Your heart rate and blood pressure have been tracked at home for decades. But one of the most revealing numbers about your health, your blood oxygen level, has only recently become easy to monitor at home. For seniors and anyone managing a chronic condition, this small number can be the difference between catching a problem early and ending up in the emergency room.
A pulse oximeter for seniors is no longer just a medical office tool. It belongs in the home health kit alongside the blood pressure cuff.
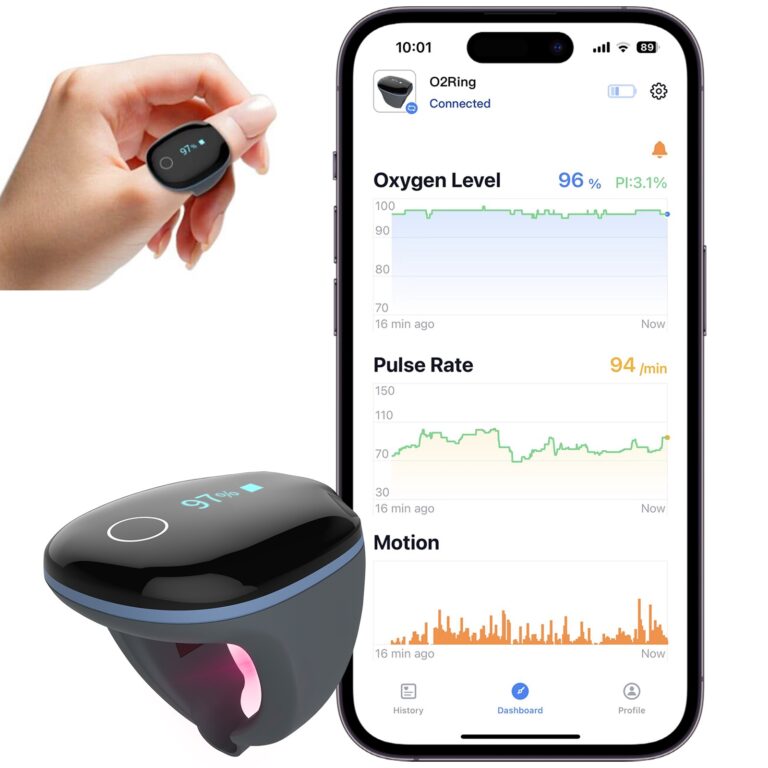
Wellue O2Ring
Wearable ring for continuous overnight oxygen monitoring with vibration alerts
Check Price on AmazonWhat Is Blood Oxygen and Why Does It Matter?
Blood oxygen saturation, measured as SpO2, tells you what percentage of your red blood cells are carrying oxygen. When you breathe, your lungs pull in oxygen and transfer it to hemoglobin in your bloodstream. That oxygen-loaded blood travels to your heart, brain, muscles, and every other organ that needs it to function.
A healthy SpO2 sits between 95% and 100%. Your body is remarkably good at maintaining this level under normal conditions. But when something disrupts breathing or circulation, that number drops. And when it drops low enough, organs begin to suffer, sometimes before you feel seriously unwell.
The tricky part: oxygen levels can fall significantly before obvious symptoms appear. By the time a person feels breathless or confused, the number may already be dangerously low. This is why passive monitoring, especially during sleep, is so valuable.
Who Benefits Most From Home Oxygen Monitoring
Anyone over 65 stands to benefit from knowing their baseline SpO2 and tracking it over time. But certain conditions make monitoring especially important.
COPD and Other Lung Conditions
Chronic obstructive pulmonary disease gradually reduces the lungs’ ability to exchange oxygen efficiently. People with COPD can have baseline readings lower than average and may experience sudden drops during activity, illness, or sleep. Catching a downward trend early allows for timely medication adjustments or a call to the doctor before things escalate.
Heart Failure and Cardiovascular Conditions
When the heart struggles to pump effectively, fluid can build up in the lungs, reducing oxygen absorption. Overnight monitoring can reveal patterns that correlate with worsening heart failure, sometimes days before other symptoms become obvious.
Sleep Apnea
This condition causes breathing to stop repeatedly during sleep, sometimes dozens or hundreds of times a night. Each pause causes a temporary oxygen drop. Many people with sleep apnea have no idea it’s happening. A continuous overnight reading can reveal these repeated dips and prompt a conversation with a doctor about formal sleep testing.
Post-Surgery Recovery
After surgery, especially procedures involving anesthesia or the chest and abdomen, oxygen levels need to stay in a healthy range. Monitoring at home during recovery gives both patients and family members a concrete number to watch.
Respiratory Illness
Whether it’s pneumonia, a severe flu, or COVID-19, respiratory infections can cause oxygen levels to slide. Home monitoring during illness lets you track whether things are improving or deteriorating, and gives you an objective data point to share with your healthcare provider.
Understanding Your Readings: What’s Normal, What’s Not
Knowing the numbers helps you respond appropriately rather than either panicking unnecessarily or ignoring something serious.
- 95% to 100%: Normal range for most healthy adults.
- 92% to 94%: Below normal. Contact your doctor, especially if this is lower than your usual baseline.
- Below 92%: Seek medical attention. This level can indicate serious respiratory or cardiac stress.
- Below 88%: This is a medical emergency. Call 911.
It’s worth establishing your personal baseline when you’re feeling well. Some people, especially older adults with certain conditions, naturally run slightly lower than the textbook range. Knowing your normal makes it easier to recognize when something has changed.
Context also matters. A brief dip during vigorous activity is different from a sustained low reading at rest. Repeated dips during sleep, even brief ones, deserve a conversation with your doctor.
Why a Finger Clip Isn’t Enough for Overnight Monitoring
Inexpensive finger clip oximeters have their place. They give you a quick spot-check reading in seconds, which is useful during illness or after exertion. But they have a major limitation: they only tell you the number right now.
The most important oxygen events often happen while you’re asleep. A finger clip can’t tell you what happened at 2 a.m. when your breathing paused. It can’t alert you when your levels drop below a safe threshold. And it certainly can’t send that data to your daughter in another city who’s keeping an eye on your health.
This is what sets continuous ring-style monitors apart, and it’s why the Wellue O2Ring has become the standout choice as a pulse oximeter for seniors who need more than a quick check.
The Wellue O2Ring: Continuous Monitoring That Works While You Sleep
The O2Ring is worn on the finger like a ring, not clipped on. It tracks SpO2 and heart rate continuously throughout the night, recording data the entire time you sleep. In the morning, you have a complete picture of what your oxygen levels were doing for eight hours, not just the single moment you happened to check.
Vibration Alerts for Low Oxygen
One of the most practical features is the built-in vibration alert. If your SpO2 drops below a level you’ve set, the ring vibrates gently on your finger. This can wake you just enough to take a deeper breath or shift position without fully interrupting your sleep. It’s a subtle but meaningful safeguard for anyone whose oxygen might dip during the night.
You can customize the threshold. If your doctor has told you that your baseline runs at 93%, you’d set the alert accordingly rather than using a generic number.
The App and Your Health History
The O2Ring syncs with the ViHealth app on a smartphone or tablet. The app stores your overnight reports and displays them in easy-to-read graphs. You can see your average SpO2, the lowest point reached, how many times it dipped below your threshold, and how that compares to previous nights.
This history matters. A single low reading could be a positioning fluke. A consistent pattern of dips over two weeks is information your doctor needs to see.
Sharing Data With Family and Providers
The app makes it simple to share reports. An adult child can be added to receive the data. A weekly report can be exported as a PDF and emailed to a cardiologist or pulmonologist. For families where one member is helping manage a parent’s health from a distance, this kind of remote visibility is genuinely reassuring.
It also changes conversations with healthcare providers. Rather than describing symptoms vaguely, you arrive with objective data. “Here’s my overnight report for the past three weeks” is far more actionable than “I’ve been feeling a bit off.”
Comfort for All-Night Wear
A device worn overnight needs to be comfortable enough to stay on. The O2Ring is designed with this in mind. The silicone ring comes in different sizes and fits securely without cutting off circulation or feeling uncomfortable against the skin. Most people find it easy to sleep with after the first night or two.
Sleep Apnea Screening at Home
Formal sleep apnea diagnosis requires a sleep study, either in a lab or with a home testing kit prescribed by a doctor. The O2Ring is not a diagnostic device and does not replace that process.
What it can do is give you meaningful data to bring to that conversation. If your overnight reports consistently show repeated oxygen dips, oxygen desaturation events where the number drops and recovers multiple times across the night, that’s a clear signal to ask your doctor about a sleep study.
Sleep apnea is dramatically underdiagnosed, especially in older adults. The classic picture of loud snoring and daytime exhaustion doesn’t fit everyone. Some people have quieter symptoms, including morning headaches, waking unrefreshed, and mild cognitive fog. An overnight oxygen record that shows repeated desaturations can be the evidence needed to move from “maybe I should get checked” to actually getting checked.
When to Call a Doctor Versus When to Monitor Closely
Not every dip warrants a phone call. Here’s a practical framework for thinking through what to do.
Contact Your Doctor if:
- Your reading is consistently below 95% over several days when feeling well.
- You notice a downward trend over a week or two, even if still in normal range.
- Overnight reports show frequent dips you haven’t seen before.
- You’re recovering from illness and readings aren’t improving.
- You have new symptoms alongside lower readings: increased breathlessness, swelling, fatigue.
Call 911 if:
- SpO2 drops below 88% and doesn’t recover quickly.
- You experience sudden severe shortness of breath, chest pain, or confusion alongside a low reading.
- Someone is unconscious or unresponsive with a low or unreadable reading.
Recheck in an Hour if:
- You got a single unexpected reading but feel fine and it rebounds immediately.
- The reading was taken right after exertion and was briefly lower than usual.
- Cold fingers may have affected accuracy. Warm your hands and recheck.
Limitations to Keep in Mind
The O2Ring is a wellness monitor, not a medical diagnostic device. Being clear about what it can and can’t do helps you use it wisely.
Nail polish, particularly dark or sparkly shades, can interfere with the optical sensor. So can very cold extremities, certain skin conditions, and poor circulation in the fingers. If a reading seems unexpectedly low, check these factors before concluding there’s a medical problem.
The device measures oxygen saturation and heart rate. It does not measure blood pressure, blood sugar, or respiratory rate. It cannot diagnose conditions. It is a data-gathering tool that, used correctly, gives you and your healthcare team much better information than you’d otherwise have.
Treat the data as one input among many, not as the final word. A reading that concerns you combined with symptoms that concern you is the signal to act. A concerning reading with no symptoms still deserves a follow-up call. Your own sense of how you feel remains part of the picture.
Making It Part of Your Routine
The best health monitoring tool is the one you actually use. The O2Ring makes this easy because wearing it requires almost no active effort. You put it on before bed, let it run, and check the app in the morning with your coffee.
For family members helping manage a parent’s or spouse’s health, setting up the data sharing once means ongoing peace of mind without daily check-in calls. You can see at a glance that last night’s readings were stable and move on with your day.
For the person wearing it, the vibration alert provides a subtle safety net during the hours when no one is watching. And the growing record of nightly data gives healthcare providers the longitudinal information they rarely get from brief office visits.
As a pulse oximeter for seniors, the O2Ring does something important: it turns a number that was once only measurable during a doctor’s visit into something you can track, trend, and share. That kind of continuous visibility is what turns health monitoring from reactive to proactive.
Getting Started
Setup takes about ten minutes. Download the ViHealth app, charge the ring, follow the pairing instructions, set your alert thresholds, and wear it to bed. The app will walk you through each step with clear instructions.
If you’re buying this for a parent or older loved one, consider setting it up together during a visit. Walk through the app, set the sharing permissions, and make sure they’re comfortable with the device before leaving. That first night of data will give both of you a useful baseline and, most likely, a lot of reassurance.



